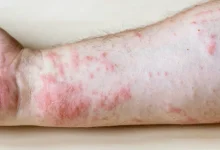
The appearance of red spots on the skin without itching can be caused by a variety of conditions and factors. These red spots can vary in size, shape, and distribution, and understanding their potential causes is crucial for determining the appropriate treatment. Below, we explore several common and less common causes of non-itchy red spots on the skin, their characteristics, and associated symptoms.
Common Causes
1. Petechiae
Petechiae are small, pinpoint, round spots that appear on the skin as a result of bleeding under the surface. They are typically red, brown, or purple and do not blanch (turn white) when pressed. Petechiae can appear in clusters and might be caused by several conditions, including:
- Physical Trauma: Minor injuries or excessive pressure on the skin can cause capillaries to burst, leading to petechiae.
- Infections: Certain infections, such as bacterial or viral infections, can lead to the development of petechiae. Notable examples include streptococcal infections and viral infections like mononucleosis.
- Medications: Some medications, particularly those that affect blood clotting, such as anticoagulants, can cause petechiae.
- Medical Conditions: Disorders affecting blood clotting or platelet function, such as thrombocytopenia (low platelet count) or leukemia, can lead to petechiae.
2. Purpura
Purpura are larger than petechiae and are caused by bleeding underneath the skin. These spots can range in size from a few millimeters to several centimeters and might appear as red or purple. Causes of purpura include:
- Vasculitis: Inflammation of blood vessels, known as vasculitis, can cause purpura. This inflammation can be due to autoimmune diseases, infections, or medications.
- Blood Disorders: Conditions that affect blood clotting or the integrity of blood vessels, such as Henoch-Schönlein purpura or idiopathic thrombocytopenic purpura, can cause purpura.
3. Allergic Reactions
Allergic reactions to medications, foods, or other substances can sometimes manifest as red spots on the skin. While itching is a common symptom of allergic reactions, it is not always present. Non-itchy red spots can appear as part of a condition called urticarial vasculitis, where inflammation of the small blood vessels leads to the formation of red patches or spots.
Less Common Causes
1. Cherry Angiomas
Cherry angiomas are benign growths made up of small blood vessels. They appear as small, round, bright red spots, typically on the trunk of the body. These lesions are usually harmless and do not cause any symptoms, although they might occasionally bleed if injured.
2. Erythema Nodosum
Erythema nodosum is an inflammatory condition characterized by the appearance of tender red nodules, usually on the shins. These nodules can be caused by a variety of factors, including infections, medications, and autoimmune diseases. Although erythema nodosum typically causes tenderness and pain, it does not always cause itching.
3. Pityriasis Rosea
Pityriasis rosea is a common, self-limiting skin condition that often begins with a single large patch known as a “herald patch,” followed by the appearance of multiple smaller red or pink spots. The exact cause of pityriasis rosea is unknown, but it is thought to be related to a viral infection. It typically resolves on its own within several weeks to months and may or may not be itchy.
Rare Causes
1. Drug Eruptions
Certain medications can cause drug eruptions, which are adverse skin reactions. These reactions can manifest as red spots or patches on the skin and may or may not be itchy. Common culprits include antibiotics, nonsteroidal anti-inflammatory drugs (NSAIDs), and anticonvulsants.
2. Systemic Conditions
Various systemic conditions can lead to the appearance of red spots on the skin. For example:
- Systemic Lupus Erythematosus (SLE): This autoimmune disease can cause a variety of skin manifestations, including red spots or a butterfly-shaped rash across the cheeks and nose.
- Kawasaki Disease: This condition primarily affects children and involves inflammation of blood vessels throughout the body. It can cause a red rash, including red spots on the skin.
Diagnostic Approach
Diagnosing the cause of non-itchy red spots on the skin involves a thorough evaluation, including:
- Medical History: Gathering information about the onset, duration, and progression of the spots, as well as any associated symptoms or triggers.
- Physical Examination: Assessing the size, shape, distribution, and characteristics of the red spots.
- Laboratory Tests: Blood tests, including complete blood count (CBC), platelet count, and coagulation tests, can help identify underlying conditions such as infections, blood disorders, or autoimmune diseases.
- Biopsy: In some cases, a skin biopsy may be performed to obtain a tissue sample for microscopic examination, which can aid in diagnosing specific skin conditions.
Treatment
The treatment of non-itchy red spots on the skin depends on the underlying cause. Here are some general approaches based on different conditions:
- Infections: If an infection is the cause, appropriate antimicrobial therapy (antibiotics or antivirals) may be necessary.
- Blood Disorders: Treatment of blood disorders may involve medications to increase platelet count, corticosteroids, or other immunosuppressive therapies.
- Vasculitis: Managing vasculitis often requires corticosteroids or other immunosuppressive medications to reduce inflammation.
- Allergic Reactions: Discontinuing the offending medication or avoiding the allergen can help resolve the skin lesions.
- Cherry Angiomas: These usually do not require treatment unless they are cosmetically concerning or prone to bleeding. Options for removal include laser therapy or electrocautery.
- Erythema Nodosum: Treatment focuses on addressing the underlying cause and may include nonsteroidal anti-inflammatory drugs (NSAIDs) for pain relief.
Conclusion
The appearance of red spots on the skin without itching can be attributed to a wide range of conditions, from benign growths like cherry angiomas to more serious systemic diseases such as systemic lupus erythematosus. Accurate diagnosis involves a comprehensive evaluation by a healthcare professional, including a detailed medical history, physical examination, and appropriate diagnostic tests. Treatment is tailored to the specific cause and may involve medications, lifestyle modifications, or other therapeutic interventions. If you notice unexplained red spots on your skin, it is important to seek medical advice to determine the cause and receive appropriate care.
More Informations

In-depth Exploration of Causes and Conditions
To further elaborate on the causes of non-itchy red spots on the skin, we will delve into a more detailed examination of the conditions previously mentioned, including additional nuances and examples where relevant.
1. Petechiae and Purpura
Petechiae and purpura are forms of bleeding under the skin but differ in size and sometimes in the underlying causes.
Petechiae
- Characteristics: Petechiae are less than 2 mm in diameter and appear as tiny red, brown, or purple dots. They can occur anywhere on the body but are often found on the lower legs.
- Causes:
- Infectious Diseases: Conditions such as meningococcemia, endocarditis, and Rocky Mountain spotted fever can cause petechiae. Viral infections like cytomegalovirus (CMV) and Epstein-Barr virus (EBV) can also be culprits.
- Physical Strain: Severe coughing, vomiting, or childbirth can cause transient petechiae due to increased venous pressure.
- Autoimmune Disorders: Diseases like systemic lupus erythematosus (SLE) and rheumatoid arthritis (RA) may lead to the formation of petechiae.
- Nutritional Deficiencies: Vitamin C deficiency (scurvy) or vitamin K deficiency can impair blood clotting, leading to petechiae.
Purpura
- Characteristics: Purpura are larger than petechiae, typically measuring 4-10 mm. They do not blanch under pressure and can vary in color from red to purple.
- Causes:
- Vasculitis: Specific types like Henoch-Schönlein purpura (IgA vasculitis) affect small vessels and can cause purpura primarily on the buttocks, legs, and feet.
- Blood Clotting Disorders: Conditions such as disseminated intravascular coagulation (DIC) and thrombotic thrombocytopenic purpura (TTP) can present with purpura.
- Medication-Induced: Drugs like anticoagulants (e.g., warfarin) and antiplatelet agents (e.g., aspirin) can lead to purpura.
2. Allergic Reactions and Drug Eruptions
Non-itchy red spots can sometimes be the result of allergic reactions or drug eruptions.
Allergic Reactions
- Characteristics: Allergic reactions typically present with itching; however, some conditions, such as urticarial vasculitis, do not itch.
- Causes:
- Medications: Antibiotics like penicillin and sulfa drugs, as well as NSAIDs, can trigger allergic reactions leading to non-itchy red spots.
- Food Allergies: Though rare, some food allergies can present with non-itchy skin manifestations.
Drug Eruptions
- Characteristics: These can range from mild rashes to severe reactions like Stevens-Johnson syndrome (SJS) or toxic epidermal necrolysis (TEN).
- Common Drugs Involved:
- Antibiotics: Penicillins, cephalosporins, and sulfonamides.
- Antiepileptics: Phenytoin, carbamazepine, and lamotrigine.
- Allopurinol: Used for gout, can cause severe drug eruptions.
3. Cherry Angiomas and Erythema Nodosum
Cherry Angiomas
- Characteristics: Small, bright red to purple papules that are generally asymptomatic. They may appear anywhere on the body but are most common on the trunk.
- Etiology: While the exact cause is unknown, cherry angiomas are associated with aging and genetic factors. They may increase in number and size with age.
Erythema Nodosum
- Characteristics: Painful, red nodules usually located on the shins, which can be accompanied by fever and joint pain.
- Causes:
- Infections: Streptococcal infections are a common cause. Other infectious agents include tuberculosis, fungal infections, and viral illnesses.
- Medications: Oral contraceptives, sulfonamides, and iodides.
- Systemic Conditions: Inflammatory bowel disease (IBD), sarcoidosis, and pregnancy can also be associated.
4. Pityriasis Rosea and Systemic Conditions
Pityriasis Rosea
- Characteristics: Begins with a herald patch, followed by a symmetrical rash that often forms a Christmas tree pattern on the trunk.
- Etiology: Thought to be related to human herpesvirus 6 (HHV-6) or HHV-7. The condition is self-limiting and usually resolves without treatment within 6-8 weeks.
Systemic Conditions
-
Systemic Lupus Erythematosus (SLE):
- Characteristics: SLE can cause a variety of skin manifestations, including the classic malar (butterfly) rash and discoid lesions. These rashes can appear as red, scaly patches or plaques.
- Associated Symptoms: Fatigue, joint pain, and organ involvement (kidneys, heart, lungs).
-
Kawasaki Disease:
- Characteristics: Acute febrile illness in children characterized by red eyes, red tongue (strawberry tongue), swollen hands and feet, and a polymorphous rash that includes red spots.
- Complications: Coronary artery aneurysms if left untreated.
Diagnostic Tools and Techniques
Accurate diagnosis of the underlying cause of red spots involves a combination of clinical evaluation and diagnostic tests.
Medical History
- Detailed History: Includes onset, duration, and progression of the rash, associated symptoms (fever, pain, systemic symptoms), and possible triggers (medications, recent infections).
- Family History: Information about family members with similar conditions can be crucial, especially for genetic disorders.
Physical Examination
- Inspection: Close examination of the morphology, distribution, and characteristics of the spots.
- Palpation: Assessing for tenderness, warmth, or induration (hardening).
Laboratory Tests
-
Blood Tests:
- Complete Blood Count (CBC): To check for platelet count, signs of infection, and anemia.
- Coagulation Tests: Prothrombin time (PT), activated partial thromboplastin time (aPTT), and platelet function tests.
- Inflammatory Markers: Erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP).
-
Serological Tests: For autoimmune markers (ANA, anti-dsDNA) and specific infections (antistreptolysin O titer for streptococcal infections).
Imaging Studies
- Ultrasound: To evaluate deeper tissues and organs if systemic involvement is suspected.
- MRI or CT Scan: In complex cases where vasculitis or systemic diseases are involved.
Skin Biopsy
- Procedure: A small sample of skin is taken under local anesthesia and examined under a microscope.
- Histopathology: Can reveal specific patterns of inflammation, vasculitis, or abnormal cell proliferation.
Management and Treatment Strategies
Effective management requires a tailored approach based on the underlying cause.
General Measures
- Avoid Triggers: For drug-induced eruptions, discontinuing the offending medication is crucial.
- Symptomatic Relief: Application of emollients, topical steroids, or nonsteroidal anti-inflammatory drugs (NSAIDs) for pain and inflammation.
Specific Treatments
- Infections: Appropriate antibiotics or antiviral medications.
- Autoimmune Disorders: Immunosuppressants or corticosteroids to reduce immune activity.
- Vasculitis: Depending on the severity, treatment may include corticosteroids, immunosuppressive drugs, or biologic agents.
- Blood Disorders: Platelet transfusions, bone marrow stimulants, or treatments targeting the underlying cause (e.g., chemotherapy for leukemia).
Monitoring and Follow-up
- Regular Check-ups: To monitor the response to treatment and adjust as necessary.
- Patient Education: Informing patients about the nature of their condition, potential triggers, and warning signs of complications.
Conclusion
The appearance of red spots on the skin without itching encompasses a broad spectrum of potential causes, from benign and self-limiting conditions to more serious systemic diseases. A thorough understanding of the patient’s medical history, a detailed physical examination, and appropriate diagnostic testing are essential to determine the underlying cause and guide treatment. While some conditions may resolve on their own or with minimal intervention, others may require comprehensive medical management and ongoing monitoring to prevent complications. Seeking medical advice when encountering unexplained skin changes is crucial for ensuring appropriate care and improving outcomes.